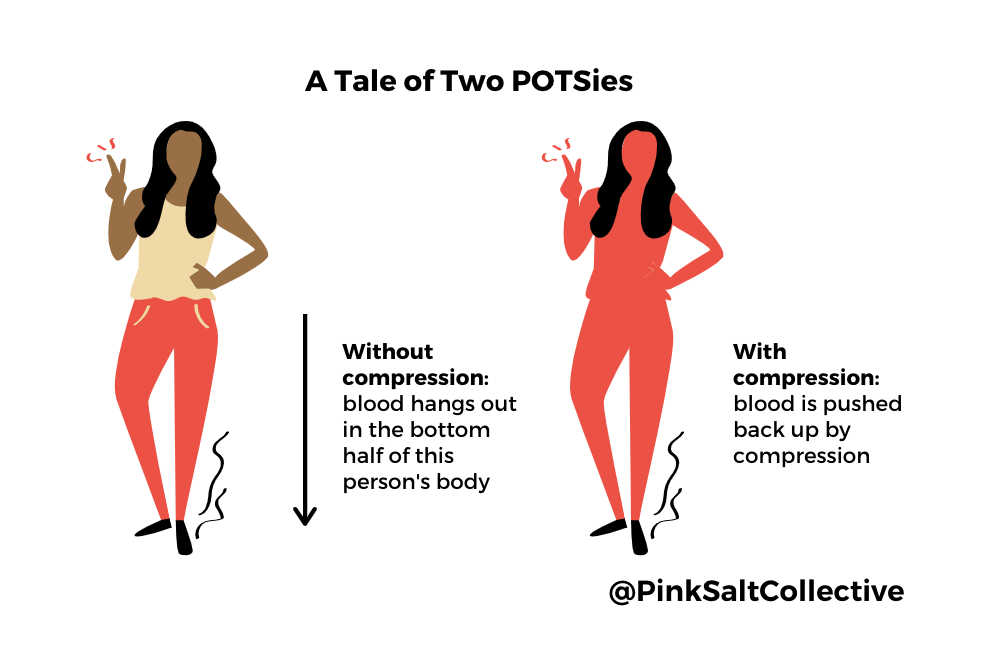MCAS stands for Mast Cell Activation Syndrome. “It’s like being allergic to everything and nothing all at once”, via @PinkSaltCollective instagram. It is an inappropriate response, or activation, of the body’s mast cells- often without a true ‘allergy’ (though people with MCAS can also have allergies and anaphylaxis).

Plenty of MCAS patients get told after allergy testing that they aren’t allergic to anything, despite having severe allergic reactions such as hives, swelling, itching, GI issues, migraines, sinusitis, etc.

Interestingly, MCAS can sometimes cause POTS or dysautonomia-type symptoms, with symptoms such as tachycardia and low blood pressure.
According to Dr. Raj, over 30% of POTS patients test positive for MCAS.
Whether this is a chicken or the egg situation, we don’t necessarily know, but it is worth noting the strong overlap in patients. For some, treating MCAS can help with POTS symptoms.
What are Mast Cells & Mediators?
Mast cells are responsible for the body’s allergic reactions. They secrete mediators such as histamine and tryptase (among others) – this process is called degranulation. During a true invasion, this helps to protect our bodies. During an MCAS episode, this degranulation is inappropriate.
Levels of these mediators can be measured as a part of testing for MCAS (blood and urine samples).
How is MCAS Tested for & Treated?
MCAS testing is sensitive and can be hard to get a ‘positive’ test during an episode. As such, many practitioners suggest that diagnosis be based on symptoms and response to therapy.
Treatment often includes: H1 blockers (such as Allegra, Zyrtec, Claritin), H2 blockers (such as pepcid), mast cell stabilizers (such as Cromolyn or Ketotifen).
Tests often include: Serum tryptase, serum histamine, 24 hour urine (N-methylhistamine, 11B -Prostaglandin F2α (11B-PGF2α) and/or Leukotriene E4 (LTE4))